We look at ways to work with pain in labour including different options for pain relief.

When it comes to giving birth, most women want to know: how much is it going to hurt and will I be able to cope with the pain? Unfortunately, you can’t answer either of these questions with certainty.
But what you can do is improve your ability to cope with pain during labour, as well as understand your options for pain relief and their impact on you, your labour and baby.
It’s not unusual for women to feel anxious and even scared of giving birth. But fear makes the body release the hormone adrenaline, and this can make contractions less efficient and slow labour down.
Pain plays a part in the process. It signals that labour has started and, as labour continues, triggers different hormones, such as endorphins, your body’s natural painkillers.
The sensations of pain change during labour and tell you that everything is progressing as it should.
Finding out about the role of hormones during labour and how you can use them to their maximum benefit can be really helpful.
You might also find it useful to read about what happens during labour, watch videos of other women giving birth and attend antenatal classes.
Your birth partner(s) will make a huge difference to how you feel during labour.
Emotional support, such as encouragement and reassurance from somebody you trust, can boost your confidence and ability to cope with pain.
It also makes sense to consider different types of pain relief. Here we look at your options…
Lying on your back can make your contractions slower and more painful. Movement, such as rocking, swaying and leaning forwards, maximises your body’s ability to give birth as it helps ease your baby along the birth canal.
Pros:
Cons:
Water can sometimes slow down labour, particularly if you get in too early.
Water soothes pain and, in a large birthing pool, supports and enables you to move into any position easily.
Pros:
Cons:
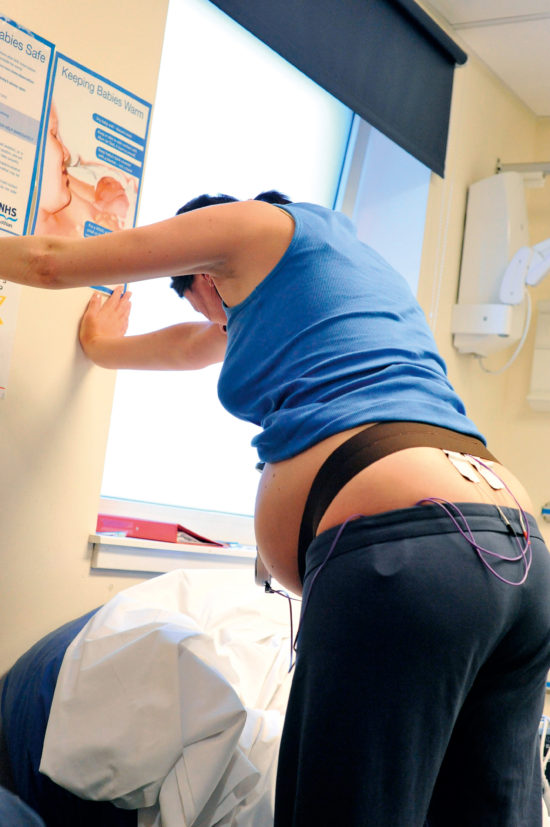
A TENS (transcutaneous electrical nerve stimulation) machine transmits mild electrical impulses to pads on your back, which block pain signals.
Pros:
Cons:
There are various complementary therapies, such as acupuncture, aromatherapy, reflexology, yoga, self-hypnosis and massage.
Pros:
Cons:
Entonox – also known as laughing gas – is a colourless, odourless gas made up of half nitrous oxide and half oxygen. You’ll probably be given gas and air through a mouthpiece and told how to breathe it in.
Pros:
It can take a few contractions to get the hang of it so that it’s effective at the peak of contractions.
Cons:
Pethidine, diamorphine and meptid are painkilling drugs given by injection into the thigh. Some hospitals offer remifentanil, which is a very strong, short acting painkiller given via a drip that you can control yourself using a machine.
All opioids pass through to your baby and can occasionally make them slower to breathe at birth. You may notice this more if your labour progresses more quickly than expected and your baby is born within two hours of your having the drug. (Effects on babies are less likely with a remifentanil infusion than they are with the other opioids because remifentanil is active in the body for a much shorter amount of time.)
Pros:
Cons:
Epidural analgesia is a local anaesthetic injected into the space between two vertebrae in your back. It usually removes all pain and most feeling from the waist down.
The combined spinal epidural (CSE) injection contains a low dose of pain-relieving drugs and works more quickly than an epidural alone. At the same time, the anaesthetist will insert a catheter. When the mini-spinal injection starts to wear off, your anaesthetist will pass the epidural solution through the tube to give ongoing pain relief.
Pros:
You may not feel contractions or – later on – the baby moving down so there is an increased chance of needing forceps or suction (ventouse) to help the baby out.
Cons:
Birth is unpredictable, but it can help to think about your different options for pain relief. Most importantly, have confidence that you can do it.
Prepare for labour and learn about birth: www.nct.org.uk/courses
Find out about our doula service and ‘Relax, stretch and breathe’ course:
www.nct.org.uk/antenatal-services
Read about pain relief: www.nct.org.uk/birth